20. januar 2022
How to stay motivated
A focus group study of Norwegian caregivers' experiences with community healthcare services to their parents with dementia

Heidi Dombestein Anne Norheim Karina Aase
Det helsevitenskapelige fakultet, UiS
heidi.dombestein@uis.no
Det helsevitenskapelige fakultet, UiS
Det helsevitenskapelige fakultet, UiS
Abstract
Motivation to provide care is a significant predictor of informal caregiving among family caregivers of persons with dementia. Adequate support is an important source of help and relief to caregivers, but fragmentation of dementia care services is common and better ways of supporting these caregivers are needed. Knowledge of adult-child caregivers’ motivation and how this motivation is influenced by community healthcare services is lacking. The aim of this study is therefore to describe and explore adult children’s experiences with community healthcare services for their home-dwelling parent with dementia and how these influence their caregiver motivation. The study applied a qualitative design based on three focus group interviews with 15 of these caregivers (40–69 years) in Norway in 2017. The study results indicate three categories supporting adult children’s sustained motivation as caregivers: (a) caregivers prioritize their parent’s need for healthcare services over their own need for support; (b) caregivers need acknowledgement through respect and involvement; and (c) caregivers need timely information and competence as the dementia progresses. To stimulate collaboration among adult-child caregivers, their parents with dementia, and community healthcare services, we claim that a relationship-centred care framework could be emphasised as a way of supporting sustained motivation among caregivers to parents with dementia as part of community healthcare services.
What is known about this topic
- Being the caregiver of a home-dwelling parent with dementia is characterised as burdensome.
- Motivation is essential for becoming and remaining engaged in the caregiver role throughout the dementia course.
- Dementia care services are fragmented and only partially successful in supporting the caregivers.
What this paper adds
- Knowledge of how adult-child caregivers’ experiences with community healthcare services influence their motivation to remain caregivers for their parent with dementia.
- Detailed descriptions of how adult-child caregivers value access to healthcare services for their parent while the caregivers are involved in a respectful way.
- A discussion of how sustained motivation among adult-child caregivers is rooted in a relationship-centred care framework.
Introduction
Dementia affects approximately 50 million persons worldwide and is one of the main causes of disability and dependency among older persons (WHO, 2020). In line with the current aging policies, the majority of older persons with dementia live as long as possible in their own homes. Although a range of community healthcare services is available to support home-dwelling parents with dementia, informal care provided by family caregivers constitutes a major portion of that care (OECD, 2018). With the need to handle a wide range of physical tasks and distressing emotional and behavioural symptoms in the home-dwelling period, caregiving has been described as progressively demanding, stressful and frustrating (Chiao et al., 2015; Yu et al., 2018). Previous research has often focused on the drawbacks of caregiving, while some studies emphasise the importance of a more balanced view (Lloyd et al., 2016) with a shift from ‘reducing stress’ to ‘optimising positive experience’ in the development of caregiving support services. Still, studies that have tried to explain the more rewarding aspects of caregiving are at a relatively early stage and the topic deserves greater attention (Lloyd et al., 2016; Yu et al., 2018).
The motivation to provide care is a significant predictor of the benefits of being a family caregiver of a person with dementia (Quinn et al., 2012; Yu et al., 2018) and has an important role in the development and maintenance of caregiving (Quinn et al., 2015). Given the challenging nature of caregiving, it is important to understand what motivates people to become caregivers for persons with dementia and especially to understand why they continue in the caregiver role, despite the growing needs of the care recipient (Greenwood & Smith, 2019). By motivation, we mean the energy in people that drives their action or inaction (Ryan & Deci, 2017; Weinstein & DeHaan, 2014).
Caregivers’ sustained motivation is influenced by factors that include individual characteristics and skills, family relations, access to health care services and the quality of those services (Greenwood & Smith, 2019; Quinn et al., 2015). Adequate formal support may provide help and relief to family caregivers and lighten the burden of caregiving (Alzheimer’s Disease International, 2018). An approach that balance the integrity of the persons with dementia with the family caregivers’ need for support is necessary in dementia care (Karlsson et al., 2015; Morrisby et al., 2018). Still, new research has found a fragmentation of dementia care services, meaning that they are only partially supporting the caregivers (Hengelaar et al., 2018; Laparidou et al., 2018). It is therefore crucial to gain knowledge of how caregivers experience community healthcare services in supporting their continued motivation for caring for persons with dementia. With the focus on interrelations among caregivers, persons with dementia, and healthcare professionals, a relationship-centred care framework that informs better ways of supporting caregivers is relevant (Nolan et al., 2003). Such relationship-centred approach should promote senses of significance, belonging, achievement, security, continuity and purpose (Nolan et al., 2001). These senses can describe the aspects of informal care often provided by family members (Wilson-Brown et al., 2013).
Caregivers of persons with dementia are a vastly diverse population. Still, most research has treated family caregivers as a homogenous group, with a few studies comparing spouse-caregivers with adult-child caregivers (Pinquart & Sörensen, 2011; Tatangelo et al., 2018). This study contributes differentiated knowledge on how adult children of parents with dementia experience community healthcare services and how these services influence their motivation to continue caregiving. The aim of this study is therefore to describe and explore adult children’s experiences with community healthcare services for their home-dwelling parent with dementia and how these influence their caregiver motivation.
Method
Study design
A qualitative design was chosen to gain insight into caregivers’ descriptions of their experiences with healthcare services when caring for home-dwelling parents with dementia. Their experiences are embedded in and formed by their social contexts (Creswell & Creswell, 2018). The study used focus group interviews to describe the caregivers’ experiences with healthcare services, leading to a deeper understanding through interactions and discussions (Morgan, 1997). The 32-item COREQ checklist is used in reporting the study (Tong et al., 2007).
Context
Like that of other Nordic countries, Norway’s public welfare model is constructed to take care of persons with dementia with supplements from informal caregivers (Norwegian Ministry of Health & Care Services, 2015). Specialist care is provided by regional health services and consists of hospitals and specialised units such as memory clinics and geriatric hospital wards. Norwegian municipalities are through community healthcare services responsible for primary care like general practitioners, home care, day-care centres and nursing homes (Norwegian Ministry of Health & Care Services, 2018). The informal care provided by adult children to parents with dementia includes for example assistance with practical tasks, transportation, support for personal care and medical treatment, but mostly emotional support, including spending time talking with the parent, visiting or calling to ensure that he or she is safe (Norwegian Ministry of Health & Care Services, 2015). According to national legislation, healthcare professionals in the community are obligated to give information, training and support to caregivers with especially onerous tasks (Health Personnel Act, 1999; Municipal Health Services Act, 2011). The Norwegian national guidelines for dementia care recommend services for persons with dementia and their caregivers to be person-centred, holistic and well-coordinated. Most of the support offered to caregivers takes the form of general information, courses in caregiving and respite stays in day-care centres and nursing homes (Norwegian Directorate of Health, 2018). The participants in this study had home-dwelling parents with dementia. They lived in urban areas or rural districts in different parts of a large municipality in western Norway.
This study is part of a PhD project, where a previous study focused on caregivers’ individual motivational drivers (Dombestein et al., 2020). Caregivers’ experiences with healthcare services are explored in this focus group study. A sample of participants from the first study volunteered to join the focus group interviews.
Recruitment procedure
Purposive sampling (Polit & Beck, 2018) was used to select participants who shared certain characteristics and had the potential to provide rich, relevant and diverse data. To be included in the study, the participants had to be over 18 years old and registered as a primary or secondary caregiver of a parent diagnosed with dementia receiving healthcare services in the municipality. Adult daughters and sons who met the inclusion criteria were identified and recruited by a project nurse working as a coordinator in the community. She was instructed to recruit both male and female caregivers. She telephoned 31 caregivers. Five declined to participate, citing limited time or energy. Author HD called the participants who had agreed to be contacted, and 21 were interviewed individually (Dombestein et al., 2020). Of those, 15 agreed to participate in the focus group interviews.
Data collection procedures
A semistructured interview guide (Malterud, 2012a, 2012b) with open-ended questions was developed with three main themes (see Table 1). The three themes were based on information required through the preceding individual interviews in which participants were asked to describe support structures that influenced their motivation to continue caring for their parents. Their responses were summarised and formed the basis for the contents of the interview guide.
TABLE 1. Interview guide with three main themes and belonging illustrative questions

The data collection was conducted over a 2-month period in 2017, and the focus group interviews took place in a meeting room at the university. Author HD moderated all three focus groups; coauthor AN was a comoderator in two of the groups, and a research fellow in one group. HD facilitated the group discussions while the comoderators made important clarifications, and took notes on group dynamics, participant interaction and nonverbal communication (Malterud, 2012a). HD is an experienced nurse trained in interviewing and consulting older persons and their caregivers. All participants were informed that the study was part of a PhD project. In the beginning of the focus group interviews the participants appeared a bit reserved, having met only the moderator once before. After some ice-breaker questions around the table, a trusting atmosphere was established in which the participants felt comfortable discussing their experiences and expressing their opinions.
Each interview was conducted in one session that lasted 92–106 min. The same interview guide was used in all focus groups. The participants did not see the list of questions prior to the interviews to reduce the risk of predetermined responses and support an open discussion. The focus group interviews were digitally audio recorded and then transcribed verbatim by author HD. The transcripts were not returned to participants for comments; their intuitive experiences were essential for the aim of the study.
Participants
Practical concerns decided the combination of participants in each focus group; participants signed up for the time and date most suitable for them. The 15 participants were therefor randomly assigned to each of the three focus groups. Group 1 consisted of two daughters and three sons; group 2 of five daughters; and group 3 of three daughters and two sons.
A total of 10 daughters and five sons participated. None of the participants had recently been sharing a household with the care recipient, and all caregivers were also holding paid jobs. Eight of the participants had parents living alone, and in seven cases, the parent with dementia lived with her or his spouse. Table 2 shows the participants’ characteristics.
TABLE 2. Characteristics of participants, N = 15 (%)

Table 2 shows the variation in caregivers’ age, gender, education, job status and the parents’ household status.
Data analysis
Systematic text condensation was used to analyse the data as it allows focusing on the particular and contextual while abstracting data (Malterud, 2012a, 2012b). The analysis consisted of four steps:
- All authors independently read the focus group transcripts to obtain an overall impression and to identify preliminary themes. This was followed by a data analysis workshop where discussions led to revised themes.
- Author HD identified meaning units and quotes reflecting each theme and developed descriptions of code groups.
- Descriptions reflecting the code groups were discussed among all authors before reorganising, renaming and eliminating code groups. Units of meaning were then split into subgroups and the contents in each subgroup were condensed.
- The contents of the condensates were synthesised into three result categories that described caregivers’ experiences with community healthcare services to stay motivated as caregivers.
Table 3 contains an excerpt of the analytical process. The data material was organised with NVivo 12 (QSR International, 2019) to systematise and identify meaning units related to the code groups.
TABLE 3. Excerpt of the analysis process using systematic text condensation
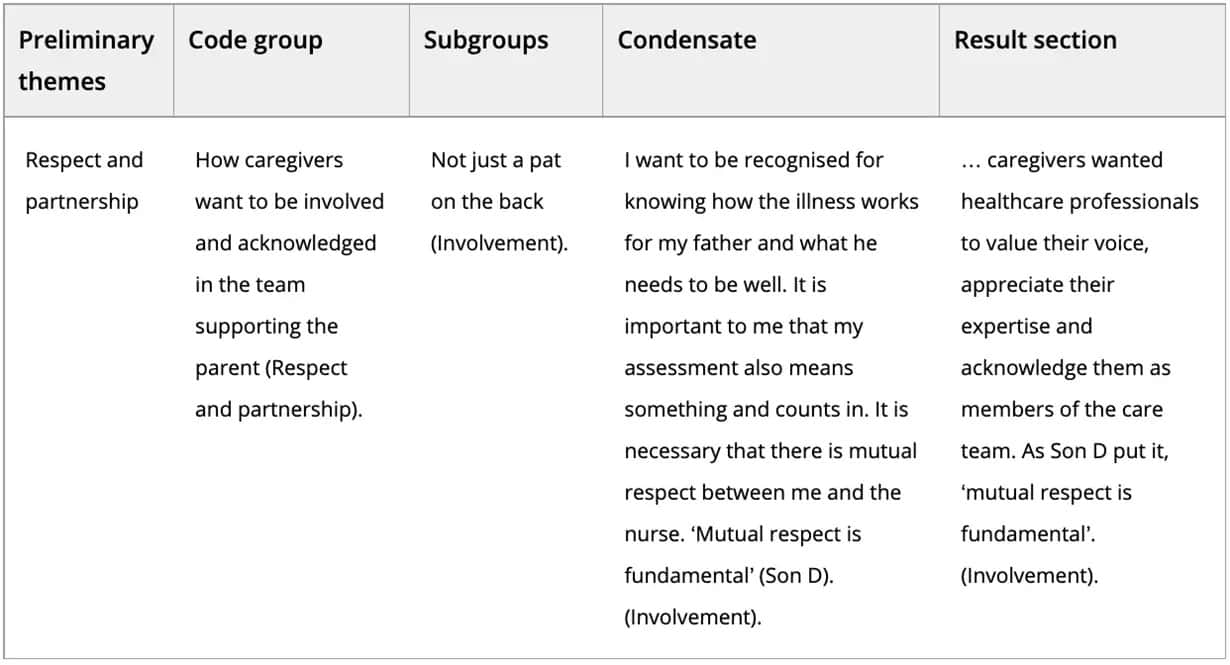
Note: Example on excerpt from the full-text section.
Ethical approval
The study was performed in accordance with the Helsinki Declaration (World Medical Association, 2008) and approved by the Norwegian Centre for Research Data (No. 48,276). All participants gave their written consent to participate and were informed that they could withdraw at any time without repercussion. They were also informed that the analysed data would be grouped so that no individuals could be identified in any reports or publications from the study.
Results
Skriv ut
Først publisert: 05.05.2021
Artikkelen er fagfellevurdert
Heidi Dombestein
Det helsevitenskapelige fakultet, UiS
heidi.dombestein@uis.no
Anne Norheim
Det helsevitenskapelige fakultet, UiS
Karina Aase
Det helsevitenskapelige fakultet, UiS
Anchor: 1
Abstract
Motivation to provide care is a significant predictor of informal caregiving among family caregivers of persons with dementia. Adequate support is an important source of help and relief to caregivers, but fragmentation of dementia care services is common and better ways of supporting these caregivers are needed. Knowledge of adult-child caregivers’ motivation and how this motivation is influenced by community healthcare services is lacking. The aim of this study is therefore to describe and explore adult children’s experiences with community healthcare services for their home-dwelling parent with dementia and how these influence their caregiver motivation. The study applied a qualitative design based on three focus group interviews with 15 of these caregivers (40–69 years) in Norway in 2017. The study results indicate three categories supporting adult children’s sustained motivation as caregivers: (a) caregivers prioritize their parent’s need for healthcare services over their own need for support; (b) caregivers need acknowledgement through respect and involvement; and (c) caregivers need timely information and competence as the dementia progresses. To stimulate collaboration among adult-child caregivers, their parents with dementia, and community healthcare services, we claim that a relationship-centred care framework could be emphasised as a way of supporting sustained motivation among caregivers to parents with dementia as part of community healthcare services.
What is known about this topic
- Being the caregiver of a home-dwelling parent with dementia is characterised as burdensome.
- Motivation is essential for becoming and remaining engaged in the caregiver role throughout the dementia course.
- Dementia care services are fragmented and only partially successful in supporting the caregivers.
What this paper adds
- Knowledge of how adult-child caregivers’ experiences with community healthcare services influence their motivation to remain caregivers for their parent with dementia.
- Detailed descriptions of how adult-child caregivers value access to healthcare services for their parent while the caregivers are involved in a respectful way.
- A discussion of how sustained motivation among adult-child caregivers is rooted in a relationship-centred care framework.
Anchor: 2
Introduction
Dementia affects approximately 50 million persons worldwide and is one of the main causes of disability and dependency among older persons (WHO, 2020). In line with the current aging policies, the majority of older persons with dementia live as long as possible in their own homes. Although a range of community healthcare services is available to support home-dwelling parents with dementia, informal care provided by family caregivers constitutes a major portion of that care (OECD, 2018). With the need to handle a wide range of physical tasks and distressing emotional and behavioural symptoms in the home-dwelling period, caregiving has been described as progressively demanding, stressful and frustrating (Chiao et al., 2015; Yu et al., 2018). Previous research has often focused on the drawbacks of caregiving, while some studies emphasise the importance of a more balanced view (Lloyd et al., 2016) with a shift from ‘reducing stress’ to ‘optimising positive experience’ in the development of caregiving support services. Still, studies that have tried to explain the more rewarding aspects of caregiving are at a relatively early stage and the topic deserves greater attention (Lloyd et al., 2016; Yu et al., 2018).
The motivation to provide care is a significant predictor of the benefits of being a family caregiver of a person with dementia (Quinn et al., 2012; Yu et al., 2018) and has an important role in the development and maintenance of caregiving (Quinn et al., 2015). Given the challenging nature of caregiving, it is important to understand what motivates people to become caregivers for persons with dementia and especially to understand why they continue in the caregiver role, despite the growing needs of the care recipient (Greenwood & Smith, 2019). By motivation, we mean the energy in people that drives their action or inaction (Ryan & Deci, 2017; Weinstein & DeHaan, 2014).
Caregivers’ sustained motivation is influenced by factors that include individual characteristics and skills, family relations, access to health care services and the quality of those services (Greenwood & Smith, 2019; Quinn et al., 2015). Adequate formal support may provide help and relief to family caregivers and lighten the burden of caregiving (Alzheimer’s Disease International, 2018). An approach that balance the integrity of the persons with dementia with the family caregivers’ need for support is necessary in dementia care (Karlsson et al., 2015; Morrisby et al., 2018). Still, new research has found a fragmentation of dementia care services, meaning that they are only partially supporting the caregivers (Hengelaar et al., 2018; Laparidou et al., 2018). It is therefore crucial to gain knowledge of how caregivers experience community healthcare services in supporting their continued motivation for caring for persons with dementia. With the focus on interrelations among caregivers, persons with dementia, and healthcare professionals, a relationship-centred care framework that informs better ways of supporting caregivers is relevant (Nolan et al., 2003). Such relationship-centred approach should promote senses of significance, belonging, achievement, security, continuity and purpose (Nolan et al., 2001). These senses can describe the aspects of informal care often provided by family members (Wilson-Brown et al., 2013).
Caregivers of persons with dementia are a vastly diverse population. Still, most research has treated family caregivers as a homogenous group, with a few studies comparing spouse-caregivers with adult-child caregivers (Pinquart & Sörensen, 2011; Tatangelo et al., 2018). This study contributes differentiated knowledge on how adult children of parents with dementia experience community healthcare services and how these services influence their motivation to continue caregiving. The aim of this study is therefore to describe and explore adult children’s experiences with community healthcare services for their home-dwelling parent with dementia and how these influence their caregiver motivation.
Anchor: 3
Methods
Study design
A qualitative design was chosen to gain insight into caregivers’ descriptions of their experiences with healthcare services when caring for home-dwelling parents with dementia. Their experiences are embedded in and formed by their social contexts (Creswell & Creswell, 2018). The study used focus group interviews to describe the caregivers’ experiences with healthcare services, leading to a deeper understanding through interactions and discussions (Morgan, 1997). The 32-item COREQ checklist is used in reporting the study (Tong et al., 2007).
Context
Like that of other Nordic countries, Norway’s public welfare model is constructed to take care of persons with dementia with supplements from informal caregivers (Norwegian Ministry of Health & Care Services, 2015). Specialist care is provided by regional health services and consists of hospitals and specialised units such as memory clinics and geriatric hospital wards. Norwegian municipalities are through community healthcare services responsible for primary care like general practitioners, home care, day-care centres and nursing homes (Norwegian Ministry of Health & Care Services, 2018). The informal care provided by adult children to parents with dementia includes for example assistance with practical tasks, transportation, support for personal care and medical treatment, but mostly emotional support, including spending time talking with the parent, visiting or calling to ensure that he or she is safe (Norwegian Ministry of Health & Care Services, 2015). According to national legislation, healthcare professionals in the community are obligated to give information, training and support to caregivers with especially onerous tasks (Health Personnel Act, 1999; Municipal Health Services Act, 2011). The Norwegian national guidelines for dementia care recommend services for persons with dementia and their caregivers to be person-centred, holistic and well-coordinated. Most of the support offered to caregivers takes the form of general information, courses in caregiving and respite stays in day-care centres and nursing homes (Norwegian Directorate of Health, 2018). The participants in this study had home-dwelling parents with dementia. They lived in urban areas or rural districts in different parts of a large municipality in western Norway.
This study is part of a PhD project, where a previous study focused on caregivers’ individual motivational drivers (Dombestein et al., 2020). Caregivers’ experiences with healthcare services are explored in this focus group study. A sample of participants from the first study volunteered to join the focus group interviews.
Recruitment procedure
Purposive sampling (Polit & Beck, 2018) was used to select participants who shared certain characteristics and had the potential to provide rich, relevant and diverse data. To be included in the study, the participants had to be over 18 years old and registered as a primary or secondary caregiver of a parent diagnosed with dementia receiving healthcare services in the municipality. Adult daughters and sons who met the inclusion criteria were identified and recruited by a project nurse working as a coordinator in the community. She was instructed to recruit both male and female caregivers. She telephoned 31 caregivers. Five declined to participate, citing limited time or energy. Author HD called the participants who had agreed to be contacted, and 21 were interviewed individually (Dombestein et al., 2020). Of those, 15 agreed to participate in the focus group interviews.
Data collection procedures
A semistructured interview guide (Malterud, 2012a, 2012b) with open-ended questions was developed with three main themes (see Table 1). The three themes were based on information required through the preceding individual interviews in which participants were asked to describe support structures that influenced their motivation to continue caring for their parents. Their responses were summarised and formed the basis for the contents of the interview guide.
TABLE 1. Interview guide with three main themes and belonging illustrative questions
The data collection was conducted over a 2-month period in 2017, and the focus group interviews took place in a meeting room at the university. Author HD moderated all three focus groups; coauthor AN was a comoderator in two of the groups, and a research fellow in one group. HD facilitated the group discussions while the comoderators made important clarifications, and took notes on group dynamics, participant interaction and nonverbal communication (Malterud, 2012a). HD is an experienced nurse trained in interviewing and consulting older persons and their caregivers. All participants were informed that the study was part of a PhD project. In the beginning of the focus group interviews the participants appeared a bit reserved, having met only the moderator once before. After some ice-breaker questions around the table, a trusting atmosphere was established in which the participants felt comfortable discussing their experiences and expressing their opinions.
Each interview was conducted in one session that lasted 92–106 min. The same interview guide was used in all focus groups. The participants did not see the list of questions prior to the interviews to reduce the risk of predetermined responses and support an open discussion. The focus group interviews were digitally audio recorded and then transcribed verbatim by author HD. The transcripts were not returned to participants for comments; their intuitive experiences were essential for the aim of the study.
Participants
Practical concerns decided the combination of participants in each focus group; participants signed up for the time and date most suitable for them. The 15 participants were therefor randomly assigned to each of the three focus groups. Group 1 consisted of two daughters and three sons; group 2 of five daughters; and group 3 of three daughters and two sons.
A total of 10 daughters and five sons participated. None of the participants had recently been sharing a household with the care recipient, and all caregivers were also holding paid jobs. Eight of the participants had parents living alone, and in seven cases, the parent with dementia lived with her or his spouse. Table 2 shows the participants’ characteristics.
TABLE 2. Characteristics of participants, N = 15 (%)
Table 2 shows the variation in caregivers’ age, gender, education, job status and the parents’ household status.
Data analysis
Systematic text condensation was used to analyse the data as it allows focusing on the particular and contextual while abstracting data (Malterud, 2012a, 2012b). The analysis consisted of four steps:
- All authors independently read the focus group transcripts to obtain an overall impression and to identify preliminary themes. This was followed by a data analysis workshop where discussions led to revised themes.
- Author HD identified meaning units and quotes reflecting each theme and developed descriptions of code groups.
- Descriptions reflecting the code groups were discussed among all authors before reorganising, renaming and eliminating code groups. Units of meaning were then split into subgroups and the contents in each subgroup were condensed.
- The contents of the condensates were synthesised into three result categories that described caregivers’ experiences with community healthcare services to stay motivated as caregivers.
Table 3 contains an excerpt of the analytical process. The data material was organised with NVivo 12 (QSR International, 2019) to systematise and identify meaning units related to the code groups.
TABLE 3. Excerpt of the analysis process using systematic text condensation
Note
Example on excerpt from the full-text section.
Ethical approval
The study was performed in accordance with the Helsinki Declaration (World Medical Association, 2008) and approved by the Norwegian Centre for Research Data (No. 48,276). All participants gave their written consent to participate and were informed that they could withdraw at any time without repercussion. They were also informed that the analysed data would be grouped so that no individuals could be identified in any reports or publications from the study.
Anchor: 4
Results
Our analysis has identified three categories that represent adult children’s experiences with community healthcare services and how these influence their motivation in caring for home-dwelling parents with dementia. First, caregivers prioritized their parent’s need for healthcare services over their own need for support. Second, caregivers needed to be acknowledged through respect and involvement. Third, caregivers need timely information and competence as the parent’s dementia progresses. Overall, the adult children painted a nuanced picture of their experiences with their parents’ healthcare services. The caregivers could cite occasions that had thwarted their motivation or experiences that sustained their motivation.
Caregivers prioritize their parent’s need for healthcare services over their own need for support
Support services specifically directed towards the caregivers were not seen as useful as long as the parent with dementia was not doing well at home. The adult children did not want their needs to be considered separately from those of their parent. It was clear that the adult children prioritised their parent’s needs over their own. It was also difficult for them to imagine the forms such support could take. Son E summarised the discussion of support for caregivers:

All the caregivers were most concerned with having the parent with dementia receive the appropriate healthcare services at the appropriate time as the dementia illness progressed. The adult children believed that they had an important role in helping connect their parent to the services they needed. Such services often started with the parent’s general practitioner (GP) diagnosing the parent with dementia and making a referral to the community coordinator who would then assign services like day-care centre, home nursing and eventually respite stays in a nursing home. Several of the caregivers regarded the GP as a gatekeeper who unlocked community healthcare services, so having a good dialogue with that GP was essential:

Most of the adult children reported varying degrees of resistance from the parent in receiving help from outside the family. This was a source of frustration and conflict between the caregiver and the parent:

A parent rejecting to receive healthcare services also included refusing to take the dementia diagnostic tests, refusing to go to the day-care centre or refusing to apply for short-term respite stays at a nursing home. Healthcare professionals often fell short in helping these parents, so the adult children had to take on those tasks themselves. Most of the adult children had been struggling to cover their parents’ need for the right healthcare services and others had received services too late. It was discouraging not feeling able to accomplish anything because their parents did not receive the healthcare services they needed. In the words of Daughter R, ‘It was like banging my head against the wall … I just wanted to give up’. In these situations, some adult children found it hard to remain motivated as caregivers. Daughter U described it this way:

Homecare nursing services were rarely described as optimal in cases where the parent was dismissive of the services or for other reasons did not receive help. The children linked the parent’s resistance to receive healthcare services to the substandard quality of the services and the fact that too many different healthcare professionals visited their parent’s home, something that felt unsafe. Most caregivers opined that homecare nursing should focus more on improving the quality of their services related to dementia competence and on workforce stability. A few of the parents had been offered homecare nursing from a smaller dementia team consisting of specially trained nurses, which worked out much better. Here, caregivers found that the assistance provided was targeted, useful and ensured continuity of services and safety for both the parents and the caregivers:

Even though the adult-child caregivers had experienced variability in the quality of services, most of them had also experienced ‘backing’ from healthcare professionals. They gave examples of receiving advice and having supportive conversations with healthcare professionals working at their parent’s day-care centre. At the same time, they knew that their parent had a good time with others and had eaten two meals that day. This gave the caregivers a sense of relief and respite. The day-care centre thus met the interconnected needs of both the adult-child caregiver and the parent. Others mentioned an alliance with the primary nurse in the homecare services where they had enjoyed dialogue and exchange of information. Daughter R gave an example:

Although the adult children saw their own needs as interconnected with those of the parent and were not concerned with support structures for their own role, they still had needs of their own as presented below.
Caregivers need acknowledgement through respect and involvement
Some of the adult-child caregivers described not having been seen, heard or respected by healthcare personnel in the community. They found it demotivating to have their knowledge or opinions disregarded, or when their consistent care for their parents seemed to have been taken for granted:

All the adult children insisted that they did not need praise or compensation for having done healthcare professionals’ tasks. They all had good relationships with their parents, and it was natural to help them. As Son E declared, ‘I don’t need a pat on the back. I really don’t appreciate that, because that is not what this is all about’. Instead, caregivers wanted healthcare professionals to value their voice, appreciate their expertise and acknowledge them as members of the care team. As Son D put it, ‘mutual respect is fundamental’. The adult children accepted that the healthcare professionals were experts on dementia, but that they knew their parents better and had the best sense of the measures that would be most helpful in difficult situations. To feel motivated, the caregivers wanted a place in the care team alongside healthcare professionals. They wanted to contribute, but not with everything all the time. The adult children understood that their mother or father could not receive unlimited healthcare services, but they sought more dialogue and interaction with the healthcare services. Son E reflected on this issue:

Caregivers need timely information and competence as the dementia progresses
One of the main reasons for the adult-child caregivers’ motivation was to ensure that their parent could have the best possible life and to receive the help he or she needed. To provide such help, caregivers required more information and advice about dementia. Some caregivers had been invited to attend a ‘caregiver school’, but only a few had participated. Some had not been aware of the services and other did not have the time or energy. Most caregivers had seen it as essential to search information online themselves or talk to people in their private network who had competence in dementia and/or how to navigate in the healthcare system. Daughter N explained how she missed information:

All of the adult children wanted to get the accurate and timely information, and to ensure their parent’s access to needed services. Caregivers also wanted specific information such as what to expect with their parent’s type of dementia, disease development, and functional ability in order to make informed decisions:

The adult children wanted to be considered as capable partners in their parent’s healthcare services. Several of them understood that this would require a better knowledge of dementia. A daughter explained that she had learned an incredible amount about dementia and how it affected her mother. As a result, she remained motivated, involved and engaged in the healthcare services. It was also clear that the caregivers expected healthcare professionals to have expertise on dementia when working with their parents:

The adult-child caregivers agreed that such competence among caregivers and healthcare personnel would constitute a win-win situation for everyone involved in caring for the parent with dementia.
Discussion
Our study of adult-child caregivers’ experiences with community healthcare services for their home-dwelling parents with dementia found that the caregivers stayed motivated if their parent’s needs for healthcare services were sufficiently met. The caregivers saw their own needs as interconnected with those of the parent placing their parents’ needs first. Furthermore, they wanted to be involved as respected and competent members of the community healthcare team.
The adult-child caregivers in our study were motivated by healthcare professionals’ respect and wanted to be involved partners in the community healthcare team. They also wanted their specific competence on the needs and possible measures for their parent to be acknowledged. According to the relationship-centred care framework (Nolan et al., 2003), this is in line with the sense of significance, a feeling of being recognised and heard. The emphasis on involvement and being part of the parent’s healthcare team is also indicative of the sense of belonging. This implies a feeling of being part of something, to be able to maintain relationships, and not being ‘in this alone’ (Nolan et al., 2003). The adult children in our study wanted professionals to have expertise on the dementia of their parent and also in how to collaborate with caregivers. Laparidou et al. (2018) found that lack of training of healthcare professionals led to absence of information for caregivers and thus did not fully support the caregivers as part of the services. Hengelaar et al. (2018) described professionals who were not confident or qualified to support informal caregivers in a partnership. The caregivers in our study appreciated their own and professionals’ competence in dementia as contributing for better help for their parent. Such a sense of achievement implies a feeling of ‘getting somewhere’, to meet challenges and competing demands, and to develop new skills (Nolan et al., 2003).
Even if the adult children in our study wanted to be partners in the community healthcare services, not all caregivers do. Spouses and others who cohabit with the persons with dementia might need other forms of support to reduce the demands on caregiving (Moholt et al., 2020). The sample in our study mainly consisted of highly educated women between the age of 50 and 59 and working full-time. They should be considered as resourceful caregivers and their motivation might differ from caregivers less likely to speak up for themselves and their parents with dementia. Many of the participants had university education, with assumably higher levels of health literacy and thus higher level of satisfaction in the caregiver role (Yuen et al., 2018). Häikiö et al. (2020) therefore recommend targeted support taking caregivers’ health literacy into account increasing the potential to enhance their ability to provide sustainable care over time.
Regardless of the adult children’s competence, access to timely and appropriate services for their parent was essential to keep caregivers motivated. In situations where the adult children struggled obtaining access to services, they compared it to ‘banging their head against a wall’. They emphasised the value of being secured that their parent’s needs were met at an early stage. This sense of security makes caregivers feel confident, able to provide good care, having adequate support networks, and timely healthcare services when required (Nolan et al., 2003). Security was achieved through receiving high-quality services at the right time from the dementia team. Variability in the quality of services is nevertheless confirmed by the caregivers of our study, as well as in other studies (Tretteteig et al., 2019). High-quality services also produced a sense of continuity through the use of a limited number of professionals working in the healthcare team and collaborating closely with the adult-child caregivers. Continuity implies the provision of competent and consistent standards of care (Nolan et al., 2003). Professionals can thus provide security and continuity by clarifying goals, consequences of actions, expectations, providing feedback, and supporting caregivers’ control, provide an overview of the situation, and plans for future tasks (Pierce et al., 2001; Tretteteig et al., 2017). The adult children in our study were more concerned with the quality of their parents’ healthcare services than their own need for support. It was hard for them to differentiate their own needs from those of their parent. The caregivers’ motive for providing care was encompassed by an overarching purpose where their parent should do as well as possible while living at home. This sense of purpose implies having goals, feeling capable of making a difference, and striking a balance between caregiving and other parts of life (Nolan et al., 2003). Community healthcare services should thus work with caregivers in a way that recognises their expertise, not supporting caregivers beyond a point at which their health suffers (Quinn et al., 2015; Nolan et al., 2003).
The relationship-centred care framework implies that good care of high quality can only be delivered when all the ‘senses’ are experienced by the persons with dementia, by the caregivers, and by the healthcare professionals. Nolan et al. (2003) acknowledge that this might be an idealistic goal in contexts where lack of resources is a reality (Hengelaar et al., 2018; Laparidou et al., 2018). Challenging relations between the person with dementia and their caregivers can also thwart caregivers’ motivation making them act out of duty (Greenwood & Smith, 2019). From the perspective of adult-child caregivers, our study results still point towards the need for continuing to strive for the senses included in relationship-centred care to support caregivers’ sustained motivation.
Limitations
We conducted three focus group interviews with 15 participants. A larger sample could have generated more information. A small sample from the Norwegian context may also affect transferability to countries dominated by private healthcare. The need for support to parents with dementia and their caregivers was reported by adult children. Asking spouses the same questions might lead to different answers. The similarity in caregiver experiences reported by the participants in the study might be caused by homogeneity in the sample, meaning that caregivers who were struggling probably declined to participate. Still, we suggest that our findings might be transferable to settings such as adult children caring for home-dwelling parents with other long-term illnesses.
Implications
Community healthcare services can optimise the positive aspects of caregiving for adult-child caregivers to persons with dementia by implementing the relationship-centred care framework that emphasises significance, belonging, achievement, security, continuity, and purpose. More research can form the basis for finding better ways of giving support tailored to the three categories that influence caregivers’ motivation.
Conclusion
The study results reveal three categories supporting adult children’s sustained motivation in their caregiver role: (a) prioritization of parents’ need for healthcare services over caregivers’ own need for support; (b) acknowledgement of caregivers through respect and involvement; and (c) timely information and competence as the dementia progresses. From the perspective of the adult-child caregivers, respected involvement (significance, belonging, achievement) and access to healthcare services for their parent (security, continuity, purpose) influenced their sustained motivation in the caregiver role. We claim that a relationship-centred care framework could be emphasised as a way of supporting sustained motivation among caregivers to parents with dementia as part of community healthcare services.
ACKNOWLEDGEMENTS
We thank the project nurse for recruiting the caregivers who participated in the study. We also thank Kristin Humerfelt, associate professor at the University of Stavanger, for being a part of the initial research group, contributing to the development of the interview guide and for comoderating one of the focus groups.
CONFLICTS OF INTEREST
The authors declare that they have no competing interests.
Referanser
Alzheimer’s Disease International. (2018). From plan to impact: Progress towards targets of the Global action plan on dementia. Retrieved from https://www.alz.co.uk/adi/pdf/from-plan-to-impact-2018.pdf?2
Chiao, C. Y., Wu, H. S., & Hsiao, C. Y. (2015). Caregiver burden for informal caregivers of patients with dementia: A systematic review. International Nursing Review, 62, 340– 350. https://doi.org/10.1111/inr.12194
Creswell, J. W., & Creswell, J. D. (2018). Research design: Qualitative, quantitative & mixed methods approaches ( 5th ed.). Sage.
Dombestein, H., Norheim, A., & Aase, K. (2020). Caring for home-dwelling parents with dementia: A qualitative study of adult-child caregivers’ motivation. Nursing Open, 7(6), 1954– 1965. https://doi.org/10.1002/nop2.587
Greenwood, N., & Smith, R. (2019). Motivations for being informal carers of people living with dementia: A systematic review of qualitative literature. BMC Geriatrics, 19, 169. https://doi.org/10.1186/s12877-019-1185-0
Häikiö, K., Cloutier, D., & Rugkåsa, J. (2020). Is health literacy of family carers associated with carer burden, quality of life, and time spent on informal care for older persons living with dementia? PLoS One, 15(11), e0241982. https://doi.org/10.1371/journal.pone.0241982
Health Personnel Act. (1999). Act of 2 July 1999 No. 64 relating to Health Personnel etc. In Norwegian: Lov 2. juli 1999 nr. 64 Lov om helsepersonell m.v. (helsepersonelloven). Retrieved from https://lovdata.no/dokument/NL/lov/1999-07-02-64?q=helsepersonell%20loven
Hengelaar, A. H., van Hartingsveldt, M., Wittenberg, Y., van Etten-Jamaludin, F., Kwekkeboom, R., & Satink, T. (2018). Exploring the collaboration between formal and informal care from the professional perspective—A thematic synthesis. Health & Social Care in the Community, 26, 474– 485. https://doi.org/10.1111/hsc.12503
Karlsson, S., Bleijlevens, M., Roe, B., Saks, K., Martin, M. S., Stephan, A., Suhonen, R., Zabalegui, A., & Hallberg, I. R.; on behalf of the RightTimeCarePlace Consortium. (2015). Dementia care in European countries, from the perspective of people with dementia and their caregivers. Journal of Advanced Nursing, 71, 1405– 1416. https://doi.org/10.1111/jan.12581
Laparidou, D., Middlemass, J., Karran, T., & Siriwardena, A. N. (2018). Caregivers’ interactions with health care services – Mediator of stress or added strain? Experiences and perceptions of informal caregivers of people with dementia – A qualitative study. Dementia, 18, 2526– 2542. https://doi.org/10.1177/1471301217751226
Lloyd, J., Patterson, T., & Muers, J. (2016). The positive aspects of caregiving in dementia: A critical review of the qualitative literature. Dementia, 15, 1534– 1561. https://doi.org/10.1177/1471301214564792
Malterud, K. (2012a). Fokusgrupper som forskningsmetode for medisin og helsefag. (Focus groups as a research method for medicine and health sciences). Universitetsforl.
Malterud, K. (2012b). Systematic text condensation: A strategy for qualitative analysis. Scandinavian Journal of Public Health, 40, 795– 805. https://doi.org/10.1177/1403494812465030
Moholt, J.-M., Friborg, O., Henriksen, N., Hamran, T., & Blix, B. H. (2020). Non-use of community health-care services – An exploratory cross-sectional study among family care-givers for older, home-dwelling persons with dementia. Ageing and Society, 1– 25, https://doi.org/10.1017/S0144686X2000015X
Morgan, D. (1997). Focus groups as qualitative research (Vol. 2). SAGE Publications.
Morrisby, C., Joosten, A., & Ciccarelli, M. (2018). Do services meet the needs of people with dementia and carers living in the community? A scoping review of the international literature. International Psychogeriatrics, 30, 5– 14. https://doi.org/10.1017/S1041610217001491
Municipal Health Services Act. (2011). Act of 24 June 2011 No. 30 relating to Municipal Health and Care Services. In Norwegian: Lov 24. juni 2011 nr. 64. Lov om kommunale helse- og omsorgstjenester m.m. (helse- og omsorgstjenesteloven). Retrieved from https://lovdata.no/dokument/NL/lov/2011-06-24-30?q=lov%20om%20kommunale%20helse%20og
Nolan, M., Davies, N., & Grant, G. (2001). Working with older people and their families. Open University Press.
Nolan, M., Grant, G., & Keady, J. (2003). Partnerships in family care. McGraw-Hill Education.
Norwegian Directorate of Health. (2018). Nasjonal faglig retningslinje om demens (The Norwegian national guidelines for dementia care). Retrieved from https://www.helsedirektoratet.no/retningslinjer/demens
Norwegian Ministry of Health and Care Services. (2015). Dementia plan 2020 – A more dementiafriendly society. Retrieved from https://www.regjeringen.no/contentassets/3bbec72c19a04af88fa78ffb02a203da/dementia_-plan_2020_long.pdf
Norwegian Ministry of Health and Care Services. (2018). Meld. St. 15 (2017–2018) Leve hele livet – En kvalitetsreform for eldre. (Report no.15 (2017-2018). To live the whole life, a quality reform for people of old age). Retrieved from https://www.regjeringen.no/no/dokumenter/meld.-st.-15-20172018/id2599850/
OECD (Organization for Economic Cooperation and Development). (2018). Care needed – Improving the lives of people with dementia. Retrieved from http://www.oecd.org/health/care-needed-9789264085107-en.htm
Pierce, T., Lydon, J. E., & Yang, S. (2001). Enthusiasm and moral commitment: What sustains family caregivers of those with dementia. Basic & Applied Social Psychology, 23, 29– 41. https://doi.org/10.1207/S15324834BASP2301_3
Pinquart, M., & Sörensen, S. (2011). Spouses, adult children, and children-in-law as caregivers of older adults: A meta-analytic comparison. Psychology and Aging, 26, 1– 14. https://doi.org/10.1037/a0021863
Polit, D. F., & Beck, C. T. (2018). Essentials of nursing research: Appraising evidence for nursing practice ( 9th ed.). Wolters Kluwer.
QSR International. (2019). NVIVO 12 for Windows. NVIVO Web Page. Retrieved from https://qsrinternational.com/nvivo/home
Quinn, C., Clare, L., & Woods, R. T. (2012). What predicts whether caregivers of people with dementia find meaning in their role? International Journal of Geriatric Psychiatry, 27, 1195– 1202. https://doi.org/10.1002/gps.3773
Quinn, C., Clare, L., & Woods, R. T. (2015). Balancing needs: The role of motivations, meanings and relationship dynamics in the experience of informal caregivers of people with dementia. Dementia, 14, 220– 237. https://doi.org/10.1177/1471301213495863
Ryan, R. M., & Deci, E. L. (2017). Self-determination theory: Basic psychological needs in motivation, development, and wellness. Guilford Press.
Tatangelo, G., McCabe, M., Macleod, A., & You, E. (2018). “I just don’t focus on my needs”. The unmet health needs of partner and offspring caregivers of people with dementia: A qualitative study. International Journal of Nursing Studies, 77, 8– 14. https://doi.org/10.1016/j.ijnurstu.2017.09.011
Tong, A., Craig, J., & Sainsbury, P. (2007). Consolidated criteria for reporting qualitative research (COREQ): A 32-item checklist for interviews and focus groups. International Journal for Quality in Health Care, 19, 349– 357. https://doi.org/10.1093/intqhc/mzm042
Tretteteig, S., Thorsen, K., & Rokstad, A. M. M. (2019). Pårørendes Erfaringer Av Kvalitet I Helse- Og Omsorgstjenester Til Personer Med Demens Og Pårørende. En Longitudinell Narrativ Studie. (Family caregivers experiences of quality in health and care services for people with dementia and their caregivers. A longitudinal narrative study). Tidsskriftet Aldring Og Helse, 23(4), 56– 64.
Tretteteig, S., Vatne, S., & Rokstad, A. M. M. (2017). The influence of day care centres designed for people with dementia on family caregivers – A qualitative study. BMC Geriatrics, 17(5), 1– 11. https://doi.org/10.1186/s12877-016-0403-2
Weinstein, N., & DeHaan, C. R. (2014). On the mutality of human motivation and relationships. In N. Weinstein (Ed.), Human motivation and interpersonal relationships: Theory, research, and applications (pp. 3– 26). Springer Netherlands: Imprint: Springer.
WHO (World Health Organization). (2020). Dementia – Key facts. Retrieved from https://www.who.int/news-room/fact-sheets/detail/dementia
Wilson-Brown, C., Swarbrick, C., Pilling, M., & Keady, J. (2013). The senses in practice: Enhancing the quality of care for residents with dementia in care homes. Journal of Advanced Nursing, 69, 77– 90. https://doi.org/10.1111/j.1365-2648.2012.05992.x
World Medical Association. (2008). Ethical principles for medical research involving human subjects. In Declaration of Helsinki, Seoul. Retrieved from https://www.wma.net/what-we-do/medical-ethics/declaration-of-helsinki/
Yu, D. S. F., Cheng, S.-T., & Wang, J. (2018). Unravelling positive aspects of caregiving in dementia: An integrative review of research literature. International Journal of Nursing Studies, 79, 1– 26. https://doi.org/10.1016/j.ijnurstu.2017.10.008
Yuen, E. Y. N., Knight, T., Ricciardelli, L. A., & Burney, S. (2018). Health literacy of caregivers of adult care recipients: A systematic scoping review. Health & Social Care in the Community, 26(2), 191– 206. https://doi.org/10.1111/hsc.12368